Congenital heart disease (CHD) refers to a range of heart defects that are present at birth. These defects can affect the heart’s structure, its valves, blood vessels, or the chambers of the heart, impacting the heart’s ability to function properly. CHD is one of the most common birth defects worldwide, affecting millions of children and adults. Though many individuals with CHD live long and healthy lives, others may require ongoing treatment or surgery to manage symptoms and prevent complications.
This blog will explore the causes, symptoms, types, and treatment options for congenital heart disease, providing you with comprehensive insights into how this condition is diagnosed and managed.
What Causes Congenital Heart Disease?
Congenital heart disease develops during fetal development, usually during the first 8 weeks of pregnancy, when the baby’s heart and circulatory system are forming. While the exact cause is often unclear, several factors can contribute to CHD. These include:
- Genetic factors: Certain genetic conditions, like Down syndrome, can increase the risk of heart defects.
- Infections during pregnancy: Some infections, such as rubella, can interfere with the development of the fetus’s heart.
- Maternal health conditions: Diseases like diabetes, lupus, or obesity can increase the likelihood of congenital heart defects.
- Medications or drug use: Some medications, particularly during the first trimester, can increase the risk of heart defects. Alcohol and drug use can also contribute to CHD.
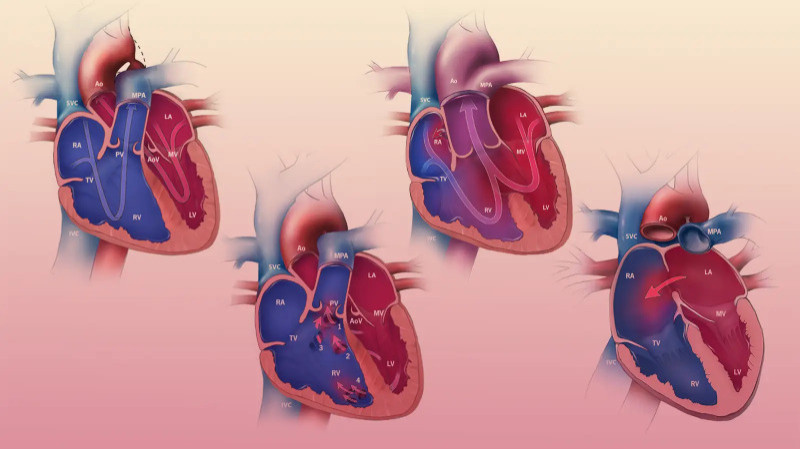
Common Types of Congenital Heart Defects
There are several types of congenital heart defects, each affecting different parts of the heart. The most common types include:
- Atrial Septal Defect (ASD): A hole in the wall between the heart’s upper chambers (atria). This condition allows oxygen-rich blood to mix with oxygen-poor blood, reducing the efficiency of the heart.
- Ventricular Septal Defect (VSD): A hole between the heart’s lower chambers (ventricles). Like ASD, this condition causes the mixing of oxygen-rich and oxygen-poor blood, leading to inefficient heart function.
- Tetralogy of Fallot: A combination of four heart defects, including a VSD, pulmonary stenosis (narrowing of the pulmonary valve), right ventricular hypertrophy (thickening of the right ventricle), and an overriding aorta. This condition restricts blood flow to the lungs and reduces oxygen levels in the blood.
- Coarctation of the Aorta: A narrowing of the aorta, the main artery that carries blood from the heart to the body. This reduces blood flow to the lower part of the body, causing high blood pressure in the arms and other complications.
- Patent Ductus Arteriosus (PDA): A condition where a blood vessel called the ductus arteriosus does not close after birth, allowing oxygenated and deoxygenated blood to mix.
- Hypoplastic Left Heart Syndrome (HLHS): A severe condition where the left side of the heart is underdeveloped, making it unable to effectively pump blood to the body. This condition is life-threatening without surgery or a heart transplant.
Symptoms of Congenital Heart Disease
The symptoms of congenital heart disease can vary depending on the severity and type of defect. While some babies with CHD may appear normal at birth, others may show signs that require immediate attention. Common symptoms include:
- Cyanosis: A bluish tint to the skin, lips, or nails due to low oxygen levels in the blood.
- Rapid breathing or difficulty breathing: Babies may breathe faster than normal or show signs of labored breathing.
- Fatigue or weakness: Children with CHD may tire easily or seem excessively tired, even after minimal activity.
- Poor feeding and slow growth: Infants may have difficulty feeding, leading to poor weight gain or slow growth.
- Swelling in the legs, abdomen, or around the eyes: This may indicate fluid buildup due to the heart’s inability to pump blood efficiently.
- Heart murmurs: A doctor may detect an abnormal heart sound (murmur) during a physical exam, which could indicate a congenital defect.
Diagnosis of Congenital Heart Disease
Diagnosing congenital heart disease typically begins with a physical examination. If a heart murmur or other abnormal signs are detected, your doctor may recommend further testing to confirm the diagnosis. Common diagnostic methods include:
- Echocardiogram: A non-invasive ultrasound of the heart that provides detailed images of the heart’s structure and function.
- Electrocardiogram (ECG or EKG): A test that measures the electrical activity of the heart, helping to detect irregular heartbeats.
- Chest X-ray: This can provide images of the heart and lungs, showing whether there are any structural abnormalities.
- MRI (Magnetic Resonance Imaging): Used to provide more detailed images of the heart and blood vessels.
- Cardiac Catheterization: In some cases, a catheter is inserted into the blood vessels to gather more information about the heart’s structure and function.
Treatment Options for Congenital Heart Disease
The treatment for congenital heart disease depends on the type and severity of the defect. While some minor defects may not require treatment, more serious conditions may need medical intervention. Here are the primary treatment options:
- Medications: Some congenital heart defects can be managed with medications to control symptoms such as irregular heart rhythms, blood pressure, or fluid buildup. Common medications include beta-blockers, diuretics, or blood thinners.
- Surgical Interventions: Many children with congenital heart disease require surgery to correct structural defects. Surgical procedures can repair holes in the heart, correct valve issues, or widen narrowed blood vessels. In some cases, multiple surgeries may be required as the child grows.
- Catheter-based Procedures: In some instances, defects can be treated with a catheter, which is a thin tube inserted into the blood vessels. This less invasive approach can be used to close holes in the heart, widen narrowed vessels, or fix valve problems.
- Heart Transplant: For severe cases, such as Hypoplastic Left Heart Syndrome, a heart transplant may be necessary. This procedure involves replacing a damaged heart with a donor heart.
- Long-term Monitoring: Children with CHD often require lifelong follow-up care to monitor their heart health. As they grow, their heart may require adjustments, and they may need additional procedures or medications.
How to Book an Appointment with the Best Cardiologist
If your child has been diagnosed with congenital heart disease or you suspect they might be showing symptoms, it’s important to see a qualified cardiologist as soon as possible. You can book an appointment with a trusted heart specialist through platforms like Instacare to ensure that your child receives the best possible care.
Instacare allows you to easily find top-rated cardiologists in your area, read reviews, and schedule appointments at your convenience, ensuring that your child gets the medical attention they need for a healthy future.
Frequently Asked Questions (FAQs)
1. Can congenital heart disease be prevented?
While congenital heart disease cannot always be prevented, maintaining a healthy pregnancy can reduce the risk. Avoiding drugs, alcohol, and smoking, managing chronic conditions like diabetes, and seeking regular prenatal care can help lower the chances of CHD.
2. Can a child with congenital heart disease live a normal life?
Many children with congenital heart disease grow up to lead normal, healthy lives, especially with early diagnosis and appropriate treatment. However, some children may face long-term complications and may need ongoing care.
3. Are there any complications associated with congenital heart disease treatment?
As with any medical procedure, surgery or interventions for congenital heart disease carry risks, such as infection, bleeding, or complications from anesthesia. However, with advancements in medical technology, the risks associated with treatment have decreased significantly, and many children recover fully.
Conclusion
In conclusion, congenital heart disease is a serious but manageable condition. Early diagnosis and treatment can significantly improve outcomes for children and adults with CHD, allowing them to lead active and fulfilling lives. Regular check-ups with a qualified cardiologist and ongoing care are essential for managing the condition.